

The effectiveness of ‘proning’ for patients with Covid-19, and it impact on reducing mortality has gained much attention over the past year. Ministry of Health and Family Welfare (MoHFW) recently advised proning for self-care amongst patients who have tested positive for Covid-19, stating it to be extremely beneficial. Now, in the current scenario when the shortage of hospital beds, drastically increased demand for oxygen concentrators and medication, etc. is being seen, improvement in oxygen levels through proning may be very relevant to possibly reduce the necessity of hospital admission.

WHAT IS PRONING?
Lying face down is known as proning, it is a medically accepted position to improve oxygenation. If a patient’s oxygen levels drop below 94 (when measured at home on an oximeter), the patient can lie on their tummy; this position improves ventilation and enables comfortable breathing.
SIGNIFICANCE
Physical position affects the distribution and volume of air in the lungs and can have direct effects on the expansion of the lungs to permit the exchange of oxygen & carbon dioxide in the blood. In the last few years, prone positioning has been used increasingly in the treatment of patients with Acute Respiratory Distress Syndrome (ARDS) and this is now considered a simple & safe method to improve oxygenation. It is a medically accepted process that involves turning a patient with precise, safe motions, from their back onto their abdomen so that the individual is lying face down to improve breathing.
Proning is required only when the patient experiences difficulty in breathing and the SpO2 decreases below 94. Regular monitoring of SpO2, along with other signs like temperature, blood pressure, and blood sugar, is important during home isolation. Moreover, missing out on Hypoxia (compromised oxygen circulation) may lead to worsening of complications. Therefore, advice must be taken from the doctor on ways to effectively practice proning at home.
HOW TO CORRECTLY DO IT?
One may prone for up to 16 hours a day, in multiple cycles, suitable to a patient’s comfort and ability. Pillows may be adjusted slightly to alter pressure areas and for comfort. Keep a track of any pressure sores or injuries, especially around the bony prominence. If this done with a help of a caregiver:
• Place one pillow below the neck
• Place one or two pillows below the chest through the upper thighs
• Place two pillows below the shins
For self-proning:
• You will need 4-5 Pillows
• Regular alterations in lying position
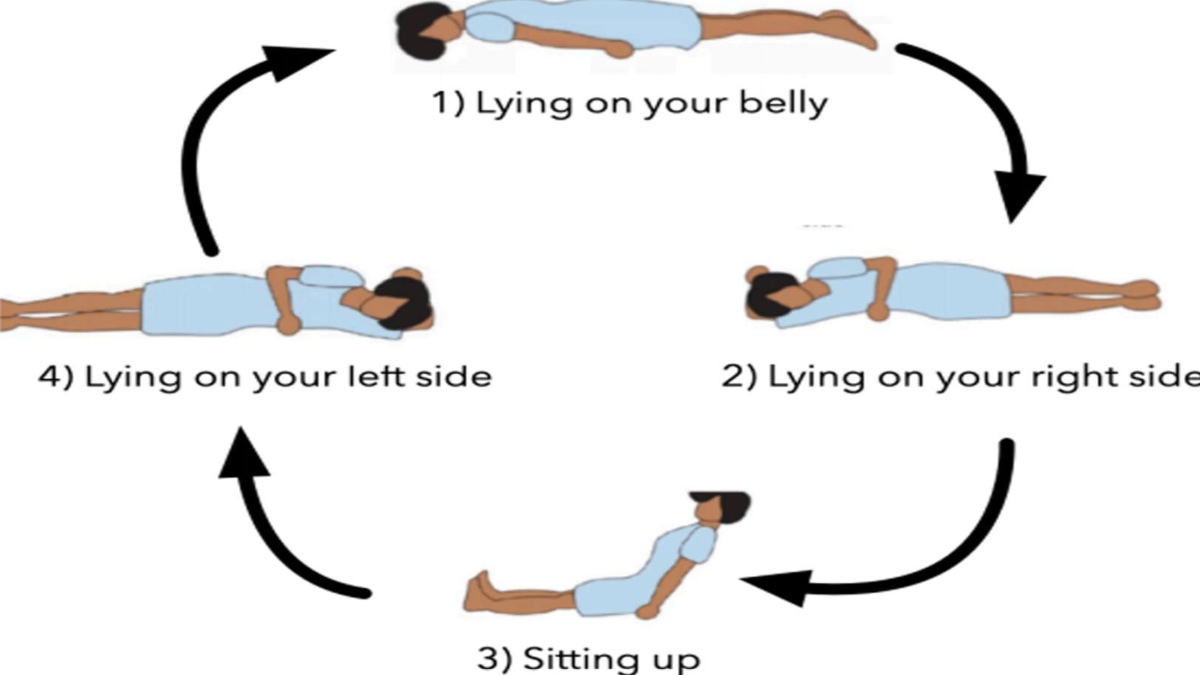
• It is best not to spend more than 30 minutes in each position, after 30 mins lie on each side, then sit up before going back to proning
What are the precautionary measures that need to be taken?
• Avoid proning if pregnant
• Avoid proning for an hour after meals
• Maintain proning for only as much time as easily tolerable
• Keep a track of any pressure sores or injuries, especially, around bony prominences
• Avoid proning if you have major cardiac conditions
• Avoid proning if you have an unstable spine, femur or pelvic fractures
The writer is an Infectious Disease Specialist at Fortis Hospital, Mulund.