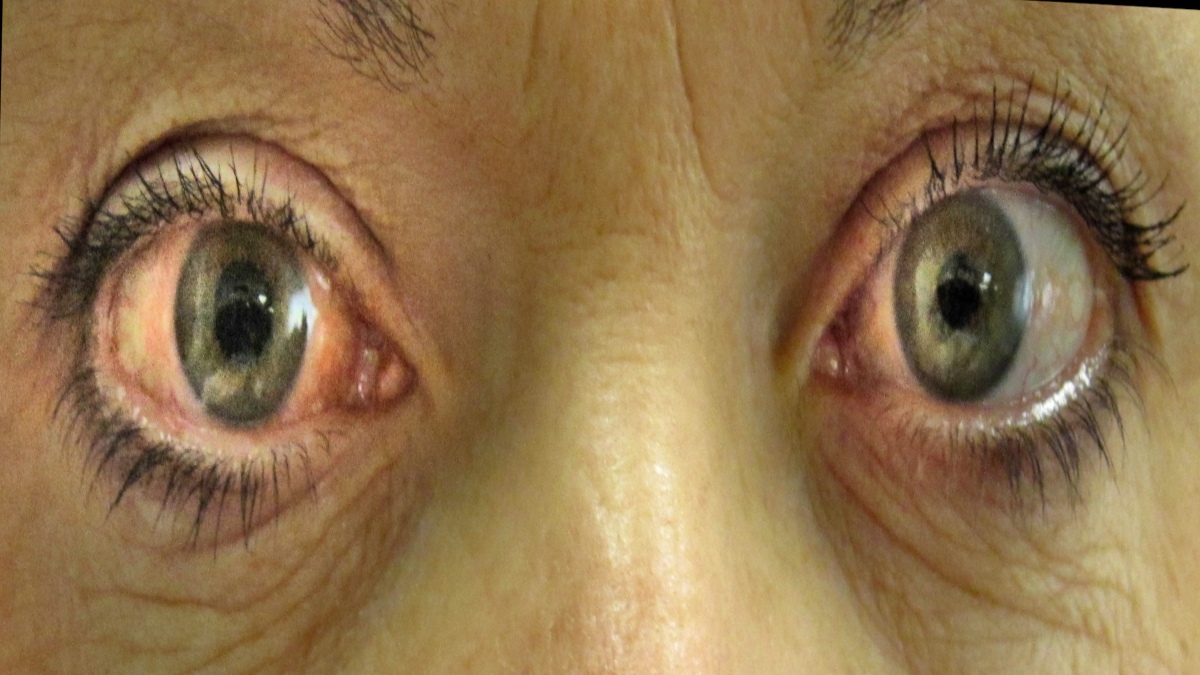
Do you know glaucoma or kala-motia is one of the leading causes of blindness? This eye disease is fairly common in adults over 35 years. If diagnosed early, blindness from glaucoma is almost always preventable.
Glaucoma afflicts over 60 million people the world over and more than half of them do not even realise it until it is too late. Rightly called the Silent Vision Stealer, this disease creeps up on unsuspecting victims and by the time it is detected, it is often too late to save the vision.
Glaucoma majorly affects the optic nerve which transmits visual messages to the brain. The nutrition to the eyes is supplied by a fluid and in normal eyes, the pressure of this fluid remains balanced. But with age, disease, trauma, or other factors, the channels carrying the fluid gets blocked, thereby increasing the pressure inside the eyes. In most cases, there are no symptoms of this increased pressure. The disease creeps in silently, first it damages the outer or peripheral vision while keeping the central vision intact. So by the time the problem is detected, the patient has already suffered extensive peripheral vision damage which is irreversible.
Three major categories of glaucoma:
1. Primary open-angle or chronic glaucoma- The most common form of glaucoma. In this, damage to the vision is gradual and generally painless.
2. Closed-angle or acute glaucoma- The intraocular pressure increases very rapidly due to a sudden and severe block of fluid drainage within the eyes. Significant symptoms indicating the presence of acute glaucoma appear immediately. This condition has to be treated quickly by an ophthalmologist otherwise may lead to blindness.
3. Other types of glaucoma- Congenital glaucoma and secondary glaucoma.
In the early stages, glaucoma generally doesn’t show any noticeable symptoms. Chronic glaucoma progresses too slowly to get noticed.
Some common symptoms of chronic glaucoma:
• Inability to adjust the eyes to darkened rooms such as theatres
• Frequent changes in eyeglass prescription
• A gradual loss of peripheral vision
• Blurred vision
• Headaches
• Poor night vision
There could be severe symptoms in the case of acute glaucoma, resulting from the rapid increase in intraocular pressure. These include:
• The feeling of a blind area in the field of vision
• Cloudy vision or seeing rainbow-coloured halos around light
• Severe eye pain, facial pain
• Red-eye
• Nausea and vomiting
Only regular eye check-ups can help catch glaucoma at a very early stage, reducing the chances of vision loss. So, everyone who is in the high-risk group should get themselves tested. People with a family history of glaucoma are at the highest risk and should get an annual test done, irrespective of their age. Others who fall in this category are people with diabetes, hypertension, thyroid, and those with a high plus or minus power.
High-risk groups who can get glaucoma:
• Family history of glaucoma
• History of diabetes
• Having high minus or plus numbered glasses
• Age above 40 years
• Having hypertension
• Anybody who has undergone any kind of eye surgery
• Having thyroid-related ailments
• Having over-mature cataracts
• Having an injury in the eye
• History of prolonged use of steroid eye drops
Points to Remember:
• There is no prevention but glaucoma is treatable
• Sometimes glaucoma symptoms are simply not noticeable
• Timely detection of glaucoma is a must
• Timely treatment of glaucoma may prevent further loss of vision and blindness.
The writer is a senior glaucoma consultant, Sharp Sight Eye Hospitals, New Delhi.